 The gold standard for diagnosing an nTOS. Therefore, it was concluded that pulse oximetry may be a quick and inexpensive tool to aide in the diagnosis of thoracic outlet syndrome (Braun et al. The EMG studies will typically show that the nerve has been injured but they dont do a good job of showing where. Oxygen saturation dropped to 86 % in the symptomatic TOS group while only dropping to 94 % in the control group. In a study by Braun and colleagues, pulse oximetry measurements in patients with symptomatic TOS were compared with measurements taken in a control group prior to and after a provocative maneuver. Blood pressure measurements in both arms, as well as auscultation of the subclavian arteries, should be performed to assess for thromboembolism or aneurysm. A sensory examination should be performed utilizing two-point discrimination and Semmes-Weinstein monofilaments, as well grip and pinch measurements. Muscle tone and bulk should be evaluated via palpation with and without resistance, especially in the neck, upper back, shoulder, arm, forearm, and hand. The skin over the chest wall, neck, and shoulder girdle should be examined for the presence of venous engorgement or collateral sprouting. 
Slouching, shoulder droop, and scapular asymmetry are clues that may lead to a diagnosis of TOS but could also represent alternative pathologies. 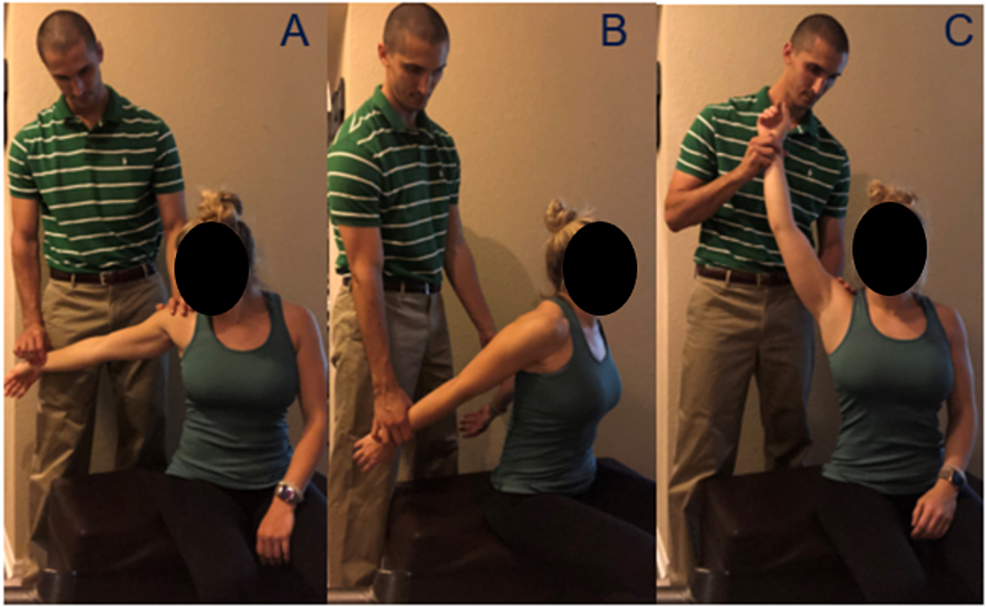
Physical examination should begin with observation of the patient’s habitus and assessment of any visible asymmetry. Although the history of patients with TOS is often nonspecific, physical examination is diagnostic in up to 97 % of patients (Rayan 1998). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
